 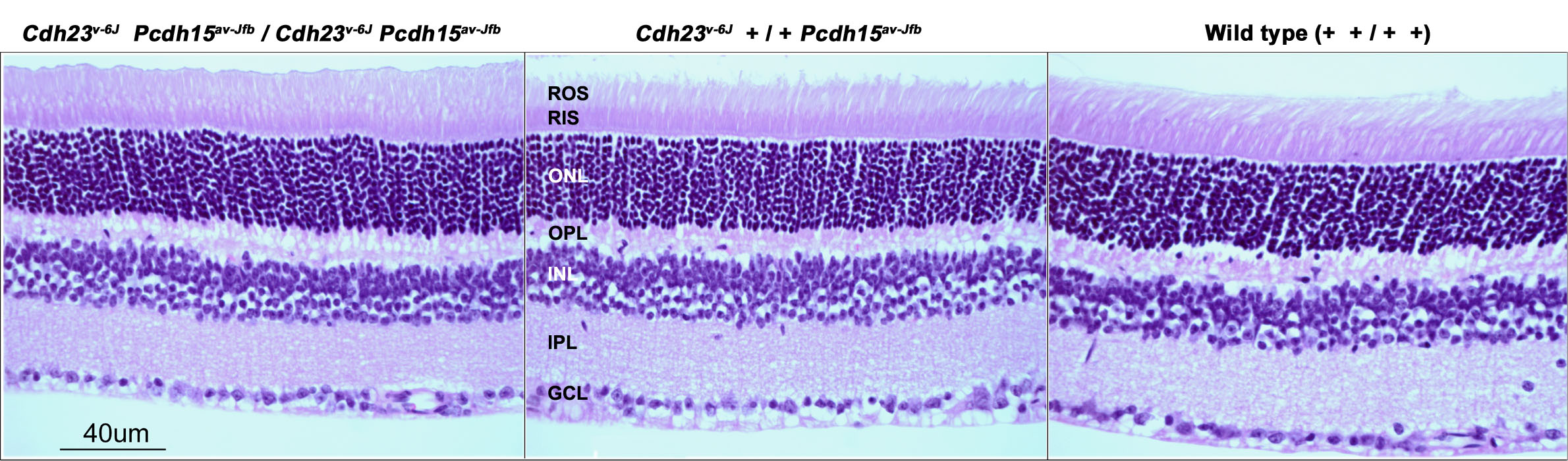
1 Abnormalities seen on OCT in this region broadly fit into the categories of thickening, thinning or simply irregular. 1 The macular choroid is typically thickest under the fovea and thinnest nasally. The normal choroidal thickness varies throughout the eye and decreases with age by 16µm per decade on average. Enhanced-depth imaging OCT and swept-source OCT are helpful in visualizing this zone, but even without them, a lot can be seen. The suprachoroidal space is a potential area between the choroid and the sclera that may become filled with fluid in certain pathologies, making it visible via OCT. Posterior to the retinal pigmented epithelium (RPE) is Bruch’s membrane, the choriocapillaris, Haller’s and Sattler’s vascular layers, then the sclera. The blue lines indicate the approximate inferior and superior margins of the nevus. Thickened choroidal nevus with posterior shadowing (red line) and overlying drusen (green line). Having a well-labeled clinical reference nearby can be helpful, both to jog our memories and for patient education ( Figure 1 ).įig. Normal StructureĪ normal macular OCT should look as familiar as the back of your hand however, remembering what structure each band on the image represents is sometimes less than second nature. Use it as a piece of the puzzle and analyze it by correlating it to the patient’s history, clinical exam and other ancillary tests when appropriate. The OCT is meant to augment your clinical exam, not replace it. Click image to enlarge.Īn accurate diagnosis cannot be made simply by comparing your OCT to similar ones on the internet. Note the larger choroidal vessels (red lines) causing choroidal thickening and inner- shifting of the RPE, and associated epitheliopathy (green line). Likewise, a serous macular detachment in central serous chorioretinopathy (CSCR) can look like a serous detachment in polypoidal choroidal vasculopathy (PCV).įig. For example, subretinal fluid (SRF) due to choroidal neovascularization (CNV) in exudative age-related macular degeneration (AMD) can resemble SRF due to CNV in myopic degeneration. Many conditions have similar pathologic features on OCT. OCT can show you some details you won’t see clinically, yet it’s important to consider OCT scans within the context of the entire clinical picture. Doing this should enable you to form several reasonable differentials based on the areas affected and better understand what’s happening and how to appropriately manage your patients. Rather, we’ll focus on critically thinking about each layered zone on a macular OCT scan, review some examples of anomalies and recognize how those abnormalities appear on OCT relative to normal structure. Click image to enlarge.įor this article, we won’t address every conceivable diagnosis. 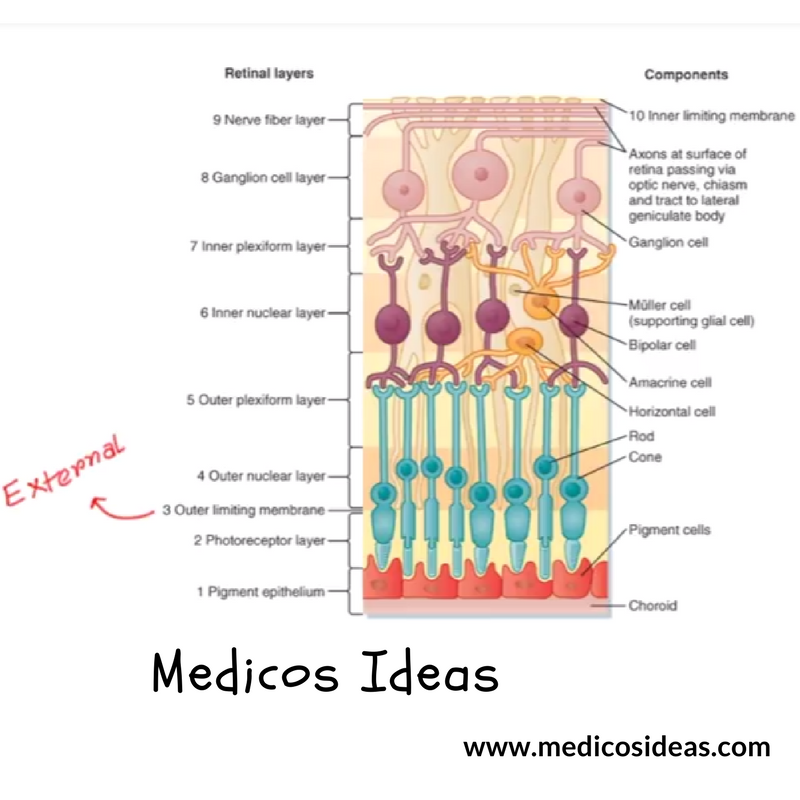 
Normal macular OCT with anatomic structures labeled. To start differentiating various macular abnormalities seen on OCT, it helps to break it into anatomic subsets, then use these groups to create differential diagnoses based on how the scan looks.įig. However, with some review and experience under your belt, you can identify what’s wrong on an OCT, correlate this with the clinical exam to make more accurate diagnoses and then begin to get more comfortable managing many of these patients on your own.Īccurate diagnosing will improve with a solid understanding of normal anatomy, then recognition of various patterns of abnormality. Interpreting an abnormality on a macular optical coherence tomography (OCT) image can be daunting for practitioners relatively new to OCT. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
